Living well with pain can be misunderstood to mean that pain won’t change or go away, or having to put up with it and that nothing can be done. This is not what it means! Pain can and does change, nothing is ever the same even though it may feel like it is. For some people pain eventually goes away and for others it doesn’t, yet it changes, and the suffering can go. We know that putting life on hold to try and ‘fix’ pain does not work and that it tends to increase suffering. Suffering can relate to many things including: feeling stuck, stopping doing what matters most, a struggle with pain, or feeling lack of purpose in life.
Living well with pain means being able to do the things: that are important to you and that matter most; the things you need to do; and doing the things that look after your health & wellbeing daily (including practices that help change pain, such as nervous system calming activities, with pain in the background.
There are many aspects involved in living well with pain, these need exploring and tailoring to what is most helpful for each individual. Living well with pain and full resolution of pain (in reality the latter doesn’t happen for many people) takes time, flexible persistence, practice and compassion, to name a few of the important things.
Living well with pain needs an understanding of the changes that happen when pain persists along with an individual toolkit of things that help look after your health & wellbeing. This blog will look at some of the aspects of living well with pain (whilst it changes in the background), and how we can do what matters most. All of the aspects covered in this blog are either already blogs and resources on the Unity Physiotherapy & Wellbeing website or they will be in the future. At the end of this blog you will find a link to a pdf resource document that has a few tips for the different aspects mentioned in this blog, along with a list of resources that are I feel are helpful and use with people in clinic. This resource list is not exhaustive and there are many more (you can also find a longer list of resources on the Unity Physiotherapy website).
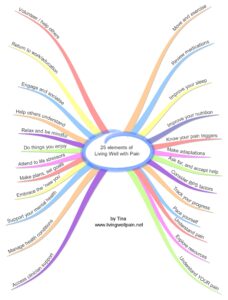
Tina, who lives with pain and runs livingwellpain.net created the helpful 25 elements of living well with pain diagram below (used here with her kind permission), and she has written about 10 of these in a blogs here http://livingwellpain.net/category/25-ways-to-manage-pain, you will find some of these woven into this blog.
Understanding Pain
Ok, this is complex! I am not going to go into the complexities of pain or the neuroscience in this blog, although understanding this and how this relates to you can be helpful. Many books delve into this in varying levels like Explain Pain & Explain Pain Supercharged (the latter is more technical read) and there are many great articles and blogs too (some are listed at the end of this blog).
Understanding the different aspects of pain can help you understand that pain is a protection mechanism and systems can become overprotective, how different systems adapt when pain persists and that they can adapt again in a helpful way. Understanding pain includes understanding why, for example, things like hurt doesn’t necessarily equal harm, pain cannot be found on scans (we are much more than a sum of our parts), pain is a protection mechanism and a poor reflection of what is going on in the tissues, movements and activities become associated with pain and are not necessarily causing harm. It’s helpful for your friends and relatives to also have an evidenced based understanding of pain and how this relates to you. An evidenced based understanding means having an awareness or a more in-depth understanding of what the research tells us about pain, and knowing what myths exist in society (there are many myths!).
(image edited, Nivens, Shutterstock)
Everything that contributes to us being human can contribute to pain, so that’s a lot of things! I would be here forever if I listed them all, to give you an idea here are some of the factors that can contribute to pain: biological factors (everything including thoughts are part of our biology), a sensitive nervous system and body (includes the immune system), not feeling safe to move, not trusting your body, beliefs, values, how we interact with the world, attention, opinions of others, previous experiences, myths about pain, expectation, self-criticism, thoughts, feelings and emotions, stress, lack of connection, avoidance, nutrition, overdoing and underdoing things, lack of purpose, feeling no-one understands, and much more.
Pacing
There is no agreed definition or set way to do this. In my mind pacing is essentially a flexible daily structure of what’s helpful for you. There are no set rules, no-one paces the same way because no-one walks in the same shoes, even though we create similar footprints. What we learn from what the evidence tells us can help, as well as from each other’s paths and footsteps. Learning how to pace and manage pain is a journey of exploration that takes many directions.
When pain persists people commonly either stop doing what matters most to them, lose purpose, or push on through things (boom-bust cycle) which commonly further sensitises things (creates more protection). I have heard it said for pacing ‘stop before you think you need a rest’, as a general rule this is not needed, although it can be part of a strategy to calm things down when you are having a flare-up or with, such as, neuropathic pain.
Have a compassionate & flexible plan as a guide when things get challenging
Life is always changing there is no constant, things are in a constant state of flux and this includes pain. Sometimes that flux changes significantly, sleep quality and function are affected, this is often referred to as a pain set-back or flare-up. It is important to know what helps when things flare-up, to help calm things back down, and approach things in a flexible and compassionate way.
Be compassionate with yourself, flare-ups are common and not a fault of anyone. Self-compassion helps in many ways including: quietening self-criticism, modulating feelings like guilt, anger and frustration, and decreasing rumination (all of these turn up the pain volume and can contribute to anxiety). Self-compassion can also help with pacing and knowing what’s helpful, as well as making wise choices that can help nurture overall health & wellbeing. It’s important to not stay at the reduced level for too long, as you will accommodate to this; this is one reason a flexible plan, that incorporates building things back up gradually, helps.
Sleep
Getting enough good quality sleep is essential for our health and wellbeing, usually this is around 7-9 hours. When living with pain, lack of sleep commonly means we notice more pain, are more sensitive to stimuli (eg react to less movement) and more easily feel stressed. There are a number of things you can do to help give yourself the best opportunity of good sleep. There are some tips in the resource accompanying this blog.
Exercise
Exercise is essential for our health and wellbeing and is helpful in living well with pain, yet there are differences in how our nervous systems and bodies react to exercise when we live with pain. Some people find exercising daunting due to significant increases in pain as a result. It is important that the exercise you do is something that you enjoy doing and you explore what is the right level to start with. Exercise is important for many reasons, even if it doesn’t modulate pain (it does for some), it helps you keep strength and tolerance to keep doing what matters.
There are a number of aspects you can modulate with exercise, like frequency, repetitions, speed, and intensity. This is a link to a blog I wrote on exercising with persistent pain, it gives some more information and general guidance https://www.unityphysio.co.uk/exercising-with-persistent-pain/. My blog and the following blog (written by physiotherapist Thomas Jesson) provide general guidance and are not intended to replace individual medical advice https://medium.com/@thomas_jesson/exercising-when-it-hurts-a8b70f7b1ebf?_referrer=twitter&fbclid=IwAR3ohbyxL7QSRzfkg1jmtHNRnxJW_ouHYD8Tm_Ql_8_88EtLBNGlPiS2pcQ
Language
What we say to ourselves (our self-talk) matters. How we talk to ourselves is a habit that we can change. Part of being human is we are wired to focus on the negative and to compare ourselves with others. We can train our language and how we relate to ourselves to be more helpful. Commonly when living with pain self-talk is often self-critical, this is part of our threat system and can contribute to systems staying on high alert which increases pain. There are some tips about language in the resource associated with this blog and more information and exercises in my pending book.
Acceptance
Acceptance is important for us all, life is tricky and we all have things to deal with that are challenging. There is a common misconception that acceptance is passive and that it means giving in or that we are happy to leave something as is, it doesn’t. It’s important to know that all any of us can do is accept things as they are in the moment, not as they will be tomorrow or next week, it’s an ongoing process not something we only do once!
Acceptance means being able to allow things to be present, with compassion, awareness and understanding, without pushing things away (avoiding), dropping the struggle and living well despite pain being present. This doesn’t mean pain won’t change, it will, instead it means pain is no longer the focus, and we are not putting life on hold waiting for the next thing that someone says will get rid of it (this commonly increases the pain and affects our mood). Instead of pain being the driver we can learn to put it in the back seat and let it be there, acceptance is one part of doing this without trying to push it out of the car (this uses so much energy and focus!). Who knows one day it may move further away and we can move it to sit on the car roof!
It’s important to remember pain can, and does, change even though for many it doesn’t fully go away it can. Acceptance helps us steer in the direction of what’s meaningful. Accepting you have persistent pain helps you take pain out of the driving seat, take back control again and steer in the direction of the things that matter to you in life even if pain is in the background.
Meaning, Purpose & Connection
One of the things, ok three things, that are particularly important are meaning, purpose and connection, these are inextricably interlinked. I have lost count of the number of times that someone has said ‘I feel like I have no purpose.’ This relates to not being connected to oneself and others, not living aligned with what’s most important (this is usually aligned to our values). By knowing what your values are and setting goals alongside these you can start to reconnect to what’s most meaningful to you. Our work can be part of our purpose and its helpful if it is, my work is connected to my purpose in life and my values.
When we stop doing what’s meaningful we lack connection to ourselves and others which is important for our wellbeing. When we do what’s meaningful to us, and when we feel connected to others, helpful neurotransmitters are released (chemical messengers) too that help modulate pain and help us feel happy, content or relaxed. Connection and compassion are both important for our wellbeing.
There is opportunity within the pain to steer towards what matters, to be guided by your values and let go of some things that don’t serve you and those around you. A lot of people say to me they are grateful in some ways as they come to see what’s most important, living with pain I can relate to this.
*This blog is intended as general information and guidance and is not intended to be individual medical advice*
Link to tips for aspects discussed in this blog
Resource alongside living well blog
Resources
Books:
- Explain Pain by David Butler & Lorimer Moseley
- Painful Yarns by Lorimer Moseley
- Pain Heros by Alison Sim
- Understand Pain Live Well Again by Neil Pearson
- The Compassionate Mind Workbook by Chris Irons & Elaine Beaumont
- Compassion focused Therapy for Dummies by Mary Welford
- The Mindful Self-Compassion Workbook by Kristin Neff & Christopher Germer.
Blogs:
- Livingwellpain http://livingwellpain.net
- My Cuppa Jo blogs https://www.mycuppajo.com
- Pain Chats https://painchats.com
Other resources:
- Pain Toolkit https://www.paintoolkit.org